Knee Injuries
The knee is an essential part of our anatomy, allowing us to stand upright, sit down, run, and engage in countless other activities. When healthy and strong, our knees work like an engineering masterpiece. If a knee injury occurs, even the most basic movements can quickly become extremely difficult, if not impossible to perform. If you’re experiencing knee pain then read on. In this post, we will discuss the basic anatomy of the knee, in addition to outlining the 3 most common knee injuries seen by physical therapists.
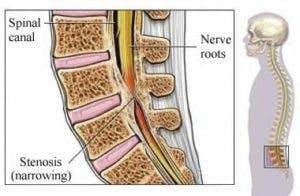
Knee Anatomy
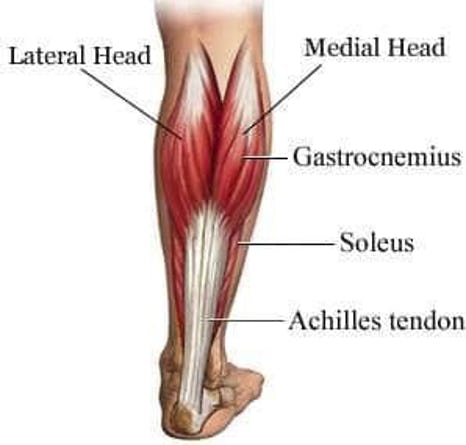
The knee joint is actually a modified hinge joint, meaning the joint allows one to flex and extend the leg, along with a small amount of internal and external (side-to-side) rotation. The entire knee joint consists of bones, ligaments, tendons, cartilage, and other vital tissues. Nearby muscles in the calf and the main supportive muscles in the upper leg — the quadriceps and the hamstrings also play a huge role in overall knee health. While any of these components could incur an injury, the 3 most common injuries are patellar tendonitis, a ligament injury (ACL, MCL, LCL, PCL), or a meniscus (cartilage) injury.
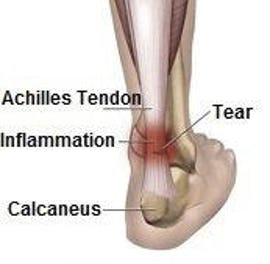
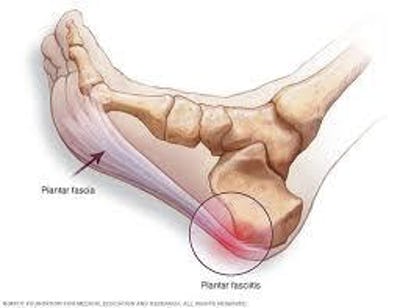
Patellar Tendonitis
This injury occurs when the tendon that connects the knee cap (patella) to the shinbone (in the calf) becomes inflamed. This injury is sometimes referred to as “jumper’s knee” as the injury often occurs from excess stress placed on the knee after landing from a jumping motion. Many athletic activities require these types of movements, and obesity can also put excess stress on this tendon as well. Pain can occur in front of, on the side, or even in the back of the knee cap. It’s very important to receive prompt medical care if a person suspects they have patellar tendonitis. Without proper treatment, the tendon is likely to become weaker and weaker, with the injured person becoming increasingly unable to perform even basic movements such as climbing stairs.
Both physicians and physical therapists have special tests they use to determine whether or not a patient may be experiencing patellar tendonitis. Once diagnosed, a physical therapist can first help by providing treatment that decreases inflammation and reduces pain. As the patient feels more comfortable a physical therapist will introduce stretching exercises, then eventually working toward strengthening exercises for surrounding muscles that help support the knee cap.

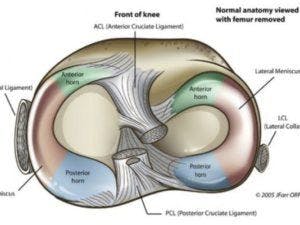
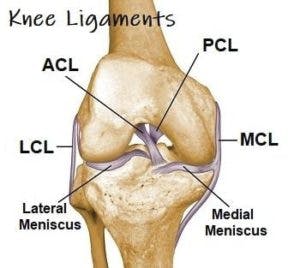
Ligament Injuries
Ligament tissues are tough, fibrous material that connects to bones — in this case, the knee bones. The 4 most common knee ligament injuries are found in the ACL (anterior cruciate ligament), the LCL ( lateral cruciate ligament), the PCL (posterior cruciate ligament) or the MCL (medial collateral ligament). All of these ligaments play a role in surrounding the knee cap and connecting it to bones in the upper leg and calf areas.
A ligament injury often manifests with sudden and severe pain, followed by knee-buckling and the inability to bear little or no weight on the injured extremity. Many patients report hearing a snap or popping sound coming from the knee when the injury first occurs. It’s important to seek immediate medical attention to determine the extent of the injury. Mild cases may require only RICE (rest, ice, compression, elevation) treatment, but more serious cases will require physical therapy and perhaps even surgery. Physical therapy goals will include working on reducing pain and inflammation, gradually increasing range of motion, and lastly, increasing strength of surrounding muscles and tissues to help support the affected ligament.
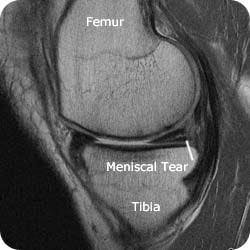
Meniscus Injury
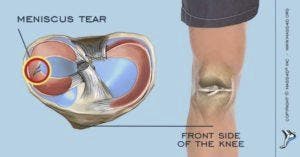
Each knee has 2 menisci — cartilage that provides cushioning between the thigh bone and the shinbone (in the calf). A tear to one of these pieces of cartilage typically occurs from a sudden pivot or rotation of the knee joint. Any athletic activity that involves sudden stop and pivot motions can result in a meniscus tear, but even heavy lifting or deep squatting can result in this type of injury as well. Knee menisci also tend to weaken with age, thus patients with knee arthritis may eventually experience a torn meniscus.
A meniscus injury will result in pain around the kneecap, especially when touched. Many patients report hearing a popping sound when the injury first occurs. Often a patient will feel as if their knee is locking or catching on something within, and they may feel as if their knee is about to buckle.
Physical Therapy Can Help
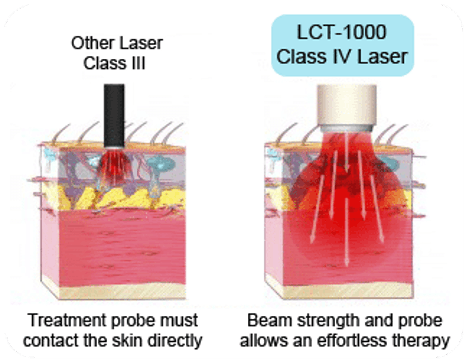
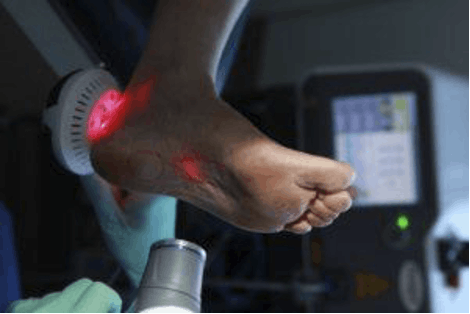
Physical therapies include effective treatments such as laser therapy, designed to reduce pain and increase healing blood flow to the area. Therapists will gradually introduce stretches designed to maintain and eventually increase range of motion, followed by strengthening exercises for muscles that support the menisci.
If you are experiencing knee pain and would like to know more about how to recover from a knee injury, please contact Hess Physical Therapy at one of our 5 locations!
Our locations:
- Kennedy: (412)-771-1055
- Crafton: (412)-458-3445
- Allison Park: (412)-487-2787
- Bethel Park: (412) 835-2626
- Atlasburg: (724) 947-9999
Website: www.hesspt.com
Disclaimer: this information is "not medical advice" and is used at the site visitor's own risk.